The Clinic Workforce We Already Have, Hiding in Plain Sight
Link Health’s New Path to Clinic Capacity and Career Pathway
The Challenge: Workforce Shortage and Patient Barriers in Tandem
According to the Harris Poll, more than half of U.S. healthcare workers plan to leave or switch jobs within the next year, underscoring a deepening crisis across hospitals, clinics, and community health settings.
Health systems and clinics are contending with interlinked problems: rising demand for social care integration, administrative burdens on staff, and decades-long workforce shortages. Many primary-care clinics are stretched thin, with frontline staff managing not only medical tasks but also the increasing demands of social-needs screening, benefit navigation, and care coordination all within a single shift.
As community health workers, nurses, physician associates, and doctors reach retirement age and fewer replacements enter the field, the pool of available support continues to shrink. This leaves a persistent challenge: building diverse, sustainable pipelines of qualified professionals equipped to serve in the healthcare sector.
Link Health’s Dual-Mission Solution
Link Health’s Patient Navigator model addresses both sides of this equation: the growing demand for social care support among patients and the staffing shortages that strain clinics.
Through our partnership with Northeastern University, pre-med, Health Science, and MPH students complete co-ops, practicums, and off-campus work-study placements with Link Health, contributing up to 200 hours in our partner clinics as trained Patient Navigators. Many go on to medical school or begin their careers at institutions such as the Colorado Department of Public Health and the Broad Institute of MIT and Harvard, and they leave our programs well prepared for their next steps because of the training and experience they gain with us.
To address increasing demand for social care services, we train emerging leaders in pre-health, public health, and social work programs to become credentialed Patient Navigators, specializing in benefits enrollment, community health integration, and patient communication. After completing this robust training, these students are deployed into clinics, transforming required service-learning or clinical hours into hands-on, direct patient-support roles.
At the same time, this workforce helps relieve overburdened clinical teams by handling many of the administrative and social-needs tasks that often fall to medical staff. The result is a sustainable, dual-mission model where health care students gain meaningful, career-advancing experience along with industry credentials and clinics gain trusted, trained support that expands their capacity to care.
Our academic partners know their scholars are receiving a structured, world-class training experience, and our clinical partners gain an adjunct workforce already aligned with their mission and workflow.
THE LINK HEALTH MODEL IN ACTION
To date, through our partnerships with several academic institutions, we have trained over 200 credentialed Patient Navigators. These emerging leaders have served at our clinical partner sites and helped over 5,000 families, unlocking over $5.2 million in support from programs such as SNAP, WIC, Medicaid/Medicare Savings, HEAP, and Lifeline.
In effect, students who might otherwise be completing shadow hours or generic internships, where they are responsible for taking coffee orders and making copies, are instead embedded in clinics serving underserved communities, performing tangible benefits navigation work that addresses the non-medical drivers of health.
In the clinic workflow, they are not passive observers; they are members of the patient’s care coordination team, screening for social needs, submitting benefits applications, tracking renewals, and coordinating case management. This support allows clinical staff to devote more time to the essential medical and relational aspects of care.
Chinoye, a Tisch Scholar at Tufts University and one of our Senior Patient Navigators, shared that she entered the role with only a foundational understanding of social determinants of health. But working directly with families quickly deepened that knowledge. Hearing firsthand how housing instability, limited access to care, and other systemic barriers shaped people’s lives made health equity feel urgent and tangible, she explained.
When asked what she’d tell another student considering the role, her answer was simple: “This work matters. You’re helping families put food on the table, keep the lights and heat on, access childcare, and feel supported,” she said. Beyond the paperwork, it’s about connection—listening to people’s stories, offering comfort, and celebrating small wins. “That’s what truly matters.”
Student + Clinic = Credit, Pay, Purpose
Our deal is simple: partner with universities whose pre-health, nursing, social work, public health, PA, OT/PT, or other programs require direct-service hours or a practicum. We then train and embed students in clinics for those hours. Students receive academic credit, structured training, and a stipend when they serve as Senior Patient Navigators. At the same time, clinics receive trained, reliable support that helps keep their patients covered, in care, and effectively managed.
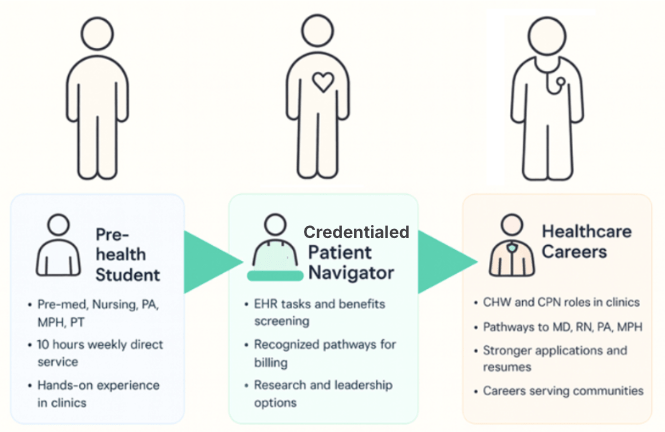
Credentialing and Career Pathways
We train students to become credentialed Patient Navigators skilled in the competencies and knowledge base through a Centers for Medicare & Medicaid Services (CMS)-approved curriculum grounded in national standards for community health integration and supervised, hands-on practice, often under the guidance of clinical professionals. These navigators are auxiliary clinical personnel who can complete defined tasks within the electronic medical records systems, screen and coordinate benefit applications and enrollment, manage documentation, and track outcomes. For students, this is far more than a one-semester stint. It offers a bridge into health careers: some go on to physical therapy, medical, nursing, or physical therapy programs; others are hired directly into community health-worker or navigator roles. Our aim is to widen the pipeline of skilled staff without lowering the bar for care.
One of our Patient Navigators, Rishi, who was recently accepted to medical school, shared that his time at Link Health gave him both the skills and confidence he needed to take that next step. He described the experience as fundamental to his journey and has since committed to supporting other aspiring, and especially non-traditional, students pursuing medicine.
Link Health Patient Navigators Can Leverage New Billing Pathways
In 2024, CMS introduced new G codes—G0019 and G0022—that allow billing for community health integration services. At Link Health, we leverage our CMS-approved credentialed Patient Navigators and have partnered with clinical sites to activate these codes, enabling Medicare reimbursement at approximately $90 per hour. This unlocks a new revenue stream for our healthcare partners while offering hands-on, real-world experience for navigators. With cost-effective labor and high-impact service delivery, this model represents a win for patients, clinics, and the growing workforce at the heart of health equity.
Clinic and System Benefits
Above and beyond the fiscal benefits, clinics gain capacity they can afford and retain because Link Health Patient Navigators absorb the high-volume, non-licensed tasks that otherwise consume the time of clinicians and front-desk staff. They help reduce lapses in benefits by keeping patients covered and engaged in care. They free professional staff to focus on what only they can do: diagnosis, treatment planning, and complex case management. The result: better-managed panels, fewer missed follow-ups, improved continuity, and stronger revenue capture where applicable.
Why Policymakers and Health Systems Should Care
If you believe in talent pipelines, budget discipline, and practical solutions, you should invest in this model. The Link Health approach uses existing institutions—universities, clinics, benefits systems—and existing opportunities. It converts mandated student hours into measurable outcomes. It builds a diverse pipeline of highly trained emerging leaders into health professionals. It supports overtaxed clinics without adding onerous new mandates. Furthermore, it creates a lasting impact by strengthening both the care workforce and the communities they serve.
Invitation to Partner
If you facilitate coursework at a university program that requires service hours, we can align those hours with patient outcomes and navigator roles. If you manage a clinic or health system, we can help you launch the Link Health Patient Navigator corps to lighten workloads today and strengthen the pipeline for tomorrow’s workforce. If you shape policy or workforce strategy, we can collaborate to scale innovative training models that expand access to care and create meaningful career pathways.
The journeys of navigators like Chinoye and Rishi show what becomes possible when we invest in emerging leaders who begin by helping patients access care and go on to transform how that care is delivered.www.link-health.org